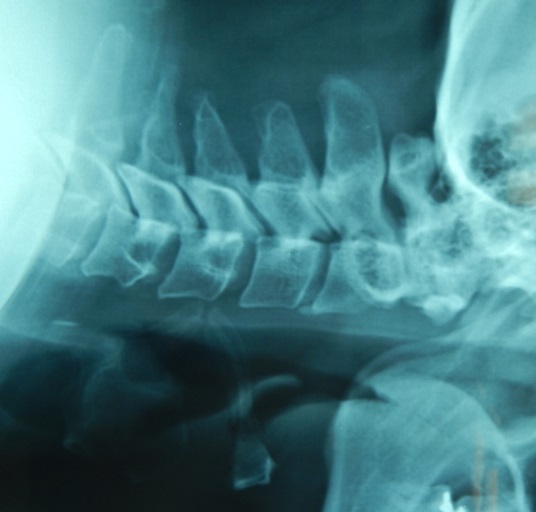
Cervical Spine in Rheumatoid Arthritis
Fuente
Este artículo es originalmente publicado en:
https://youtu.be/t-NNF5IHJfI
De y Todos los derechos reservados para:
Courtesy: Prof Nabil Ebraheim,
University of Toledo, Ohio, USA
Dr. Ebraheim educational animated video illustrates spine concepts associated the cervical spine – rheumatoid arthritis.
Cervical spine involvement occurs in about 90% of the patients with rheumatoid arthritis.
All rheumatoid arthritis patients should have cervical spine examination.
Start with getting cervical spine x-rays, because this helps to diagnose atlantoaxial instability.
Early aggressive medical treatment can decrease this risk.
C1-C2 instability is common and can occur in up to 80%.
It occurs due to transverse ligament pathology.
So you will need to get flexion extension views in patients with rheumatoid arthritis, especially preoperative x-rays, and if it looks bad, you have to stabilize the spine before doing elective total hip or total knee procedures.
Discover the C1-C2 instability and fix it first before doing elective total hip procedure.
You see in the x-rays the Atlanto Dental Interval: A.D.I., if it was more than 3.5 mm that means instability of the upper cervical spine may be present.
If it is more than 7 mm it means disruption of the alar ligament, these patients can have cervical spine myelopathy.
The A.D.I. is an unreliable predictor of paralysis.
The posterior atlanto dental interval is a better predicting test, it can predict the spinal cord injury better.
If the posterior A.D.I. is less than 14 mm it can predict spinal cord injury, get an MRI.
The surgery is done if the A.D.I. is more than 10mm or if the P.A.D.I. is less than 14mm, the operation is C1-C2 fusion.
Clinically: the C1-C2 instability could give neck pain, headache, and myelopathy with abnormal gait, paresthesia and difficulty in fine motor control.
Basilar Invagination:
Occur in about 40% of the patients with rheumatoid arthritis, basilar invagination is superior migration of the odontoid so the tip of the odontoid is above the foramen magnum; in this case you do occiput to C2 fusion, plus or minus odontoid resection.
The Subaxial Subluxation:
Occur in about 20% of the patients.
Indication of surgery is neurological compromise.
The space available for the cord is less than 14 mm then do posterior fusion surgery; surgery is usually not successful in severe types of neurological impairment.
When do you do surgery in rheumatoid arthritis?
You do it if there is:
• Severe pain
• Neurological deficit
• X-ray showing that the P.A.D.I. is less than 14mm
• Superior odontoid migration
• Subaxial subluxation and the sagittal canal diameter is less than 14 mm.
If the posterior atlanto- dental interval (P.A.D.I.) is more than 14 mm, the patient will demonstrate significant motor recovery after surgery.
Follow me on twitter:
https://twitter.com/#!/DrEbraheim_UTMC
Donate to the University of Toledo Foundation Department of Orthopaedic Surgery Endowed Chair Fund:
https://www.utfoundation.org/foundati…